Low vision is a common visual disorder in children, which seriously affects their visual perception and motor function development and brings many inconveniences to their life and learning. The application of somatosensory technology in rehabilitation provides a new opportunity for the motor function rehabilitation of children with low vision. However, the rehabilitation effect is affected by many factors. Therefore, in-depth study of these influencing factors and building an effective prediction model are of great significance for optimizing the rehabilitation program and improving the rehabilitation effect. In this study, although the somatosensory technique was effective in the rehabilitation training for children with low vision, some children still failed to achieve the ideal rehabilitation effect, suggesting that we need to further explore the factors affecting the rehabilitation effect to improve the overall success rate of rehabilitation.
The results showed that the long course of disease was an independent factor affecting the rehabilitation of children with low vision. For children with a long course of disease, long-term visual impairment may lead to more severe impacts on the development of motor function and more complex adaptive changes in the neuromuscular system, thus increasing the difficulty of rehabilitation8. For example, long-term low vision may cause children to form incorrect postures and exercise patterns during exercise, which are difficult to correct in a short time, thus affecting the effectiveness of rehabilitation training. In addition, with the prolongation of the course of disease, children may have psychological problems, such as inferiority complex and anxiety, which affect their enthusiasm and compliance to participate in rehabilitation training, and then have a negative impact on the rehabilitation effect. Training frequency and gender remained significant in both univariate and multivariate analyses. Higher training frequency may enhance motor learning opportunities, while gender differences could reflect variations in developmental trajectories or activity preferences, as observed in previous pediatric rehabilitation studies.
In clinical practice, for children with a long course of disease, more attention should be paid to the development of personalized rehabilitation program, appropriate extension of the rehabilitation training cycle, strengthen psychological support and counseling, to help children overcome difficulties, and gradually improve the motor function9. Low family support was identified as one of the important factors affecting the rehabilitation effect. The family is an important support system in the rehabilitation process of children, and the active participation and encouragement of family members are crucial for the rehabilitation of children. The low degree of family support may be reflected in the parents’ insufficient attention to rehabilitation training and failure to actively assist children in training, such as failing to take children to training on time, and not supervising children in auxiliary training at home10. The lack of family support may also lead to children not receiving enough emotional encouragement in the training process, which is conducive to the generation of negative emotions and reducing training compliance. On the contrary, children with high family support have more confidence and motivation in the training process, and parents can give positive feedback in time to help children to better master training skills and improve the rehabilitation effect. Therefore, clinical medical staff should strengthen communication and education with the parents of children, improve their understanding of rehabilitation training, encourage parents to actively participate in the rehabilitation process of children, and create a good atmosphere for family rehabilitation11.
The rehabilitation effect of children with complications is poorer. The common complications in children with low vision, such as strabismus and nystagmus, will further affect the visual perception and motor coordination ability of children. For example, strabismus may result in binocular visual dysfunction in children, resulting in inability to accurately determine the position and distance of objects, and deviations during motor function training. Nystagmus decreases the visual stability of children and makes it difficult to focus on the target object, thus affecting the accuracy and efficiency of training12. Complications may also increase the children’s fatigue and discomfort during training, and reduce their tolerance to training. For children with complications, complications should be actively treated while motor function rehabilitation training is carried out to improve the visual function and the overall situation of children, to improve the rehabilitation effect. At the same time, the training intensity and method should be adjusted according to the specific situation of children in the training process to avoid affecting the rehabilitation process due to the aggravation of complications13. Low training intensity has a significant effect on rehabilitation. Appropriate training intensity is one of the key factors to promote the recovery of motor function in children. Low-intensity training may not sufficiently stimulate the neuromuscular system of children to achieve effective training thresholds, which limits the improvement of motor function. For example, in balance training, if the training intensity is insufficient, the balance ability of children is difficult to be fully challenged and improved, and they cannot adapt to the more complex sports environment14. However, excessive training intensity may also lead to excessive fatigue, injury or resistance in children, which is also not conducive to recovery. Therefore, when formulating the rehabilitation training plan, the training intensity should be reasonably adjusted according to the children’s age, physical condition, basic motor ability and other factors, to ensure that the training is challenging and affordable for the children, to achieve the optimal rehabilitation effect15. At the same time, we should pay close attention to the children’s reaction in the process of training, and timely adjust the intensity of training, to avoid the impact of improper intensity on the rehabilitation process.
Rehabilitation for children with low basic visual acuity is more difficult. Vision is an important basis for children to perceive the external environment and engage in motor activities. Low basic vision will affect children’s perception and judgment of the surrounding environment, and thus affect the development of their motor function and the effect of rehabilitation training16. For example, during coordination training, children may not be able to accurately observe the movement demonstration or target object due to poor vision, resulting in decreased movement accuracy and coordination. In addition, low vision may also affect the children’s spatial orientation ability and motor response speed, increasing the complexity of rehabilitation training. For children with low basic visual acuity, the visual characteristics should be fully considered in rehabilitation training, and targeted training methods, such as the addition of auditory cues, tactile guidance and other multi-sensory stimulation, should be adopted to help children to better understand and complete the training tasks, and improve the rehabilitation effect17. The poor adaptability of somatosensory technology is also an important factor affecting the rehabilitation effect. Somatosensory technology requires children to be able to accurately control their body movements by capturing their movements in real time and transforming them into interactions in a virtual environment, so that the devices can be accurately identified. Children with poor adaptability may have problems in the accuracy of motion capture and the efficiency of task completion, resulting in inability to make full use of the advantages of somatosensory technology for effective rehabilitation training18. For example, children may be unfamiliar with the operation of somatosensory devices or lack of control ability of their own actions, which causes great deviation between the actions recorded by the device and the actual actions, and affects the accuracy and effectiveness of training feedback. During the training process, we should strengthen the training of children’s somatosensory technology adaptability, through gradually guiding, increase the number of exercises, help children familiar with and master the somatosensory technology, improve their interaction ability in the virtual environment, to better play the role of somatosensory technology in rehabilitation training.
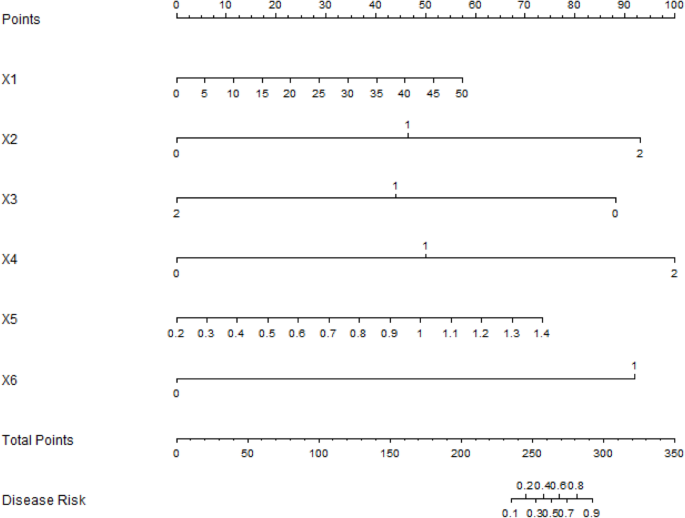
In this study, the nomogram prediction model was comprehensively evaluated based on the C-index index, calibration curve, and ROC curve. In the training set, the C-index index was 0.935, indicating that the model had high prediction accuracy and could well distinguish between effective and ineffective children undergoing rehabilitation. The C-index of the validation set was 0.841, which was slightly lower than the training set but still showed the reliability and extrapolation of the model in the new samples. The calibration curve shows that the prediction model can predict the rehabilitation effect well overall. ROC curve analysis showed AUCs of 0.941 and 0.843 for the training and validation sets, respectively, further confirming the diagnostic efficacy of the model.
The nomogram prediction model has good value in clinical application, but in the use process, the prediction results of the model need to be comprehensively analyzed in combination with the clinical actual situation, to improve the accuracy of the prediction of the rehabilitation effect of children with low vision. Clinicians can use the nomogram by locating each predictor’s value on the corresponding axis, summing the points, and translating the total into a predicted probability of ineffective rehabilitation. This can guide early intervention strategies and resource allocation. While a digital calculator was not developed for this study, such a tool could be easily created and integrated into electronic medical records for point-of-care use. Based on the model prediction results, clinicians can formulate personalized rehabilitation plan for the specific situation of children, including adjusting the training cycle, strengthening psychological intervention, collaborative treatment of complications, adjusting the training method according to the level of vision and improving the adaptability of somatosensory technology, to improve the rehabilitation effect19. Through understanding the influence of training intensity on rehabilitation effect, doctors can reasonably adjust the training intensity to avoid the adverse effect of too low or too high on the rehabilitation effect. At the same time, the physical response and motor function changes of children are closely monitored to ensure the effectiveness and safety of training.
In view of the negative influence of the course of the disease on the rehabilitation effect, the importance of early detection and timely rehabilitation training was emphasized. At the same time, the rehabilitation of children with low vision needs comprehensive treatment, including ophthalmic treatment, rehabilitation training and psychological support20. Family plays an important role in the rehabilitation of children with low vision. The results of this study emphasized the impact of family support on rehabilitation outcomes. Therefore, health education for parents should be strengthened to encourage them to actively participate in the rehabilitation training of children to form an all-round support system. This is a single-center study, and the sample size is relatively small, so there may be a certain selection bias, and the representation of the research results is limited. Future multicenter, large sample studies are needed to verify the reliability and universality of the results. In addition, the evaluation method for some influencing factors in the study may be subjective, and the evaluation method should be further optimized to improve objectivity and accuracy. In addition, the short-term rehabilitation effect was only observed in this study, and the follow-up time should be extended in future studies to evaluate the long-term rehabilitation effect and the long-term quality of life of the children21.
There some limitations in this research. (1) The definitions and sub-components of training compliance and training intensity in this study were based on clinical experience and prior small-scale practice rather than standardized, validated scales. This may limit the generalizability of our findings and should be addressed in future research. (2) In addition, this was a single-center study, which may limit generalizability. The single-center nature of the study may limit the external validity of the findings, as patient characteristics, rehabilitation resources, and clinical practices may differ across institutions and regions. (3) Some variables, such as family support, were assessed using subjective ratings, which may introduce measurement bias. Additionally, the follow-up period was limited to the short term; thus, long-term rehabilitation outcomes remain unknown.
Despite the limitations, this study still provides valuable information for the application of somatosensory technology-based motor function rehabilitation training in children with low vision. Future studies may further explore other factors that may affect the rehabilitation effect, build better prediction models, and pay attention to the application effect of new somatosensory technologies in the rehabilitation of children with low vision to provide more effective rehabilitation treatment for children22. Meanwhile, future studies should include multicenter cohorts with larger sample sizes, extend follow-up durations for longitudinal validation, and explore integrating multimodal sensor data (e.g., wearable motion sensors, eye-tracking) to enhance predictive accuracy.
link





:max_bytes(150000):strip_icc()/VWH-GettyImages-2157903338-69370a8ef92e449b8958c22cab26dd28.jpg)