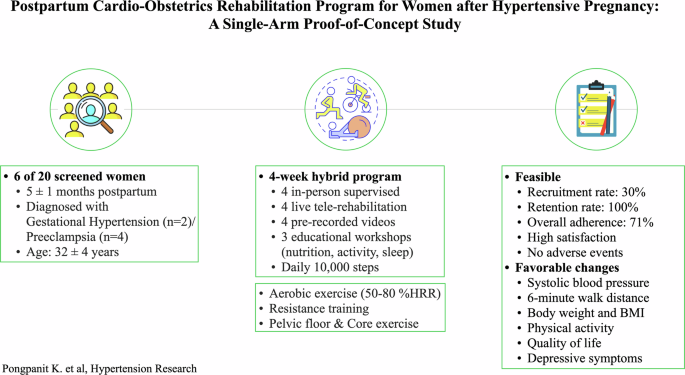
Study design
This study was designed as a pre-post single-arm proof-of-concept study. Reporting of the findings follows the CONSORT extension for pilot and feasibility trials [15]. The study was approved by the Centre Intégré Universitaire de Santé et de Services Sociaux du Nord-de-l’Île-de-Montréal (CIUSSS-NÎM) and all participants provided informed consent. Given the exploratory nature of this study, the sample size was based on feasibility, and, in line with the ORBIT model for behavioral treatment development, a control group was not required at this stage [16].
Participants
Participants were recruited between May and July 2022 from the Clinique de Grossesse à Risque at the Mother-Child Unit of the Hôpital du Sacré-Cœur de Montréal (HSCM), CIUSSS-NÎM. Eligible individuals were identified by their obstetricians, who referred those meeting the study criteria to the research team. Potential participants were then contacted by telephone, provided with detailed information about the study procedures and associated risks.
Women were eligible for inclusion if they were 18 years of age or older, between three and six months postpartum, had been diagnosed with new-onset hypertension (≥140/90 mmHg) after 20 weeks of gestation, with either the absence (gestational hypertension, GH) or presence (PE) of proteinuria or maternal organ involvement, and were not taking antihypertensive medication at the time of enrollment. Participants were also required to be able to communicate in English or French and have access to a computer or mobile device with internet connectivity. The selected postpartum timeframe aligns with typical recovery trajectories and reflects an expected period of physical and psychological readiness for re-engaging in structured physical activity, which often occurs between 8 and 12 weeks following delivery [17].
Participants were excluded if they had a diagnosis of chronic hypertension, were currently using antihypertensive medication, had major contraindications to physical activity (e.g., cardiac conditions, neurological or musculoskeletal disorders), or exhibited significant cognitive impairment or mental health conditions that could affect informed consent and study participation.
Intervention
The intervention comprised a structured, four-week cardio-obstetrics rehabilitation program integrating both exercise and educational components. The four-week duration was selected based on existing evidence suggesting that this timeframe provides sufficient opportunity for behavioral change [18] and cardiovascular adaptation to exercise [19], while remaining practical and feasible for postpartum women. Participants were expected to complete a total of 15 sessions over the intervention period, including four in-person supervised exercise sessions, four live telerehabilitation sessions, four independently completed sessions using pre-recorded videos, and three educational workshops delivered either online or in pre-recorded format. A hybrid format, combining both educational and physical components, was used to evaluate the acceptability, preference, and adherence to these different delivery methods.
Each exercise session followed a standardized structure, involving 5 min of warming up, 30 min of aerobic training, 10 min of resistance exercises, 5 min of core strengthening, 5 min of pelvic floor rehabilitation, and 5 min of stretching and relaxation. Exercise difficulty and intensity were progressively increased throughout the program. During the first week, aerobic training was performed at 50–60% of estimated heart rate reserve, increasing to 60–70% in weeks two and three, and reaching 70–80% by week four. Resistance exercise was prescribed at an intensity of 0–60% of one-repetition maximum with two to four sets of 8–12 repetitions per exercise and was adjusted based on participants’ ability and tolerance.
In-person sessions took place at the Centre Jean-Jacques-Gauthier (CJJG), CIUSSS-NÎM, and were supervised by a trained member of the research team. Aerobic training was performed using either a treadmill or stationary bike, with BP, heart rate, oxygen saturation, and perceived exertion recorded before and after each session to ensure safety and monitor physiological response. Participants were also instructed to complete one weekly telerehabilitation session delivered via Zoom under the supervision of a team member, as well as one independent session using a pre-recorded video accessed through a private YouTube channel. For both formats, they were asked to engage in 30 to 60 min of walking or aerobic activity on a self-selected day, guided by individualized targets using step counts or heart rate ranges. To facilitate self-monitoring of daily steps and exercise heart rate range and support adherence, participants were provided with a Fitbit Inspire 2 (Fitbit Inc., San Francisco, CA, USA) and a suggested daily step goal of 10,000 steps [20].
Regarding educational workshops, participants attended sessions delivered by members of the CJJG team that addressed key postpartum health topics, including nutrition, physical activity, and sleep hygiene. At the initial visit, they also received a printed leaflet outlining evidence-based physical activity recommendations for the postpartum period.
Outcome measures
Participants underwent assessments at two time points: the initial baseline visit, which took place between three to six months postpartum, and a follow-up visit after completing the four-week rehabilitation program. During the initial assessment, sociodemographic data, medical and perinatal history, and behavioral information were collected through questionnaires and review of the medical chart.
Implementation feasibility
Feasibility outcomes included recruitment, retention, adherence, acceptability, and safety. Adherence was tracked by documenting attendance at in-person and virtual sessions and reviewing completed logbooks for pre-recorded sessions. Acceptability was assessed through post-intervention feedback questionnaires. Safety was monitored by recording BP, heart rate, oxygen saturation, and perceived exertion during supervised sessions. Adverse events were defined as any unintended harmful experiences participants encountered during the intervention, which may include, but are not limited to, injuries, dizziness, fainting, severe discomfort, or other related issues [21]. These events were documented through session records and participant logs.
Quantitative physiological responses included resting BP, functional capacity, anthropometrics, and physical activity levels. Systolic and diastolic BP were measured after 10 min of seated rest using a validated automated sphygmomanometer (Omron Healthcare Co. Ltd, Kyoto, Japan). Three readings were taken at two-minute intervals, and the average of the second and third readings was used for analysis. Functional capacity was evaluated using the six-minute walk test (6MWT) following American Thoracic Society guidelines [22]. With subjects barefoot and fasted, height was measured using a wall-mounted stadiometer (Seca North America, Chino, CA, USA) and weight was measured on an electronic standing scale (Detecto, Webb City, MO, USA). Body mass index (BMI) was then calculated as weight in kilograms divided by the square of height in meters. Objective physical activity data, including step count and activity duration, were collected using a Fitbit Inspire 2, which participants were instructed to wear throughout the four-week program.
Self-reported health outcomes
Participants’ physical activity levels were also self-reported using the Pregnancy Physical Activity Questionnaire (PPAQ), while perceived functional capacity was assessed with the Duke Activity Status Index (DASI). Quality of life was measured using the 36-Item Short Form Health Survey (SF-36), and psychological well-being was evaluated using the Edinburgh Postnatal Depression Scale (EPDS) and the Patient Health Questionnaire-9 (PHQ-9).
Post-intervention feedback was collected through a custom-designed questionnaire administered via REDCap, which included both closed-ended items (5-point Likert scale) and open-ended questions. The Exercise Benefits and Barriers Scale (EBBS) was used to assess attitudes toward exercise, while perceptions of the rehabilitation process were captured using the Cardiac Rehabilitation Facilitators (CRFS) and Barriers Scale (CRBS).
Statistical analysis
Descriptive statistics were used to characterize participant demographics and outcomes. Continuous variables are reported as means with standard deviations or medians with interquartile ranges according to distribution. Changes between baseline and follow-up were reported using mean or median differences alongside effect sizes (ES) calculated with Hedges’ g, interpreted as small (0.2), medium (0.5), or large (0.8) [23]. Minimal clinically important differences (MCIDs) were employed to contextualize the clinical relevance of observed changes in physical outcomes, specifically 2 mmHg for BP [24, 25], and 30 meters for the six-minute walk distance (6MWD) [26].
link





:max_bytes(150000):strip_icc()/VWH-GettyImages-2157903338-69370a8ef92e449b8958c22cab26dd28.jpg)