
Epidemiology and clinical characteristics of AKDOPT
Between December 2017 and May 2020, the monthly cumulative incidence of AKDOPT was stable among eligible population, with the average incidence being 11.0% (95% confidence interval [CI] 10.8–11.2%), and the top 3 clinical divisions that had the highest number of AKDOPT requiring nephrology referral were cardiology, urology, and gastroenterology (Fig. 2; Supplementary Figs. 2, 3). Moreover, 23.0% (95% CI 21.9–24.0%) of the patients with AKDOPT were considered to be high risk and required nephrology referral, but only 2.8% (95% CI 2.6–2.9%) of the patients with AKDOPT actually had a nephrology clinic follow-up in the same month. In the sensitivity analyses of limiting eligible outpatient visits with at both diagnostic S-Cre measurements from CMUH’s outpatient setting or with at least one S-Cre measurements from CMUH’s outpatient, the average incidence of AKDOPT decreased to 2.9% (95% CI, 2.8–3.0%) and 6.1% (95% CI 5.9–6.3%), respectively. However, the proportion of high-risk AKDOPT remained high (32.3% [30.4–34.2%] and 28.5% [27.1–29.9%]) and the rate of AKDOPT patients having nephrology follow-up remained low (4.3% [3.8–4.8%] and 3.5% [3.3–3.7%]; Supplementary Figs. 4, 5).
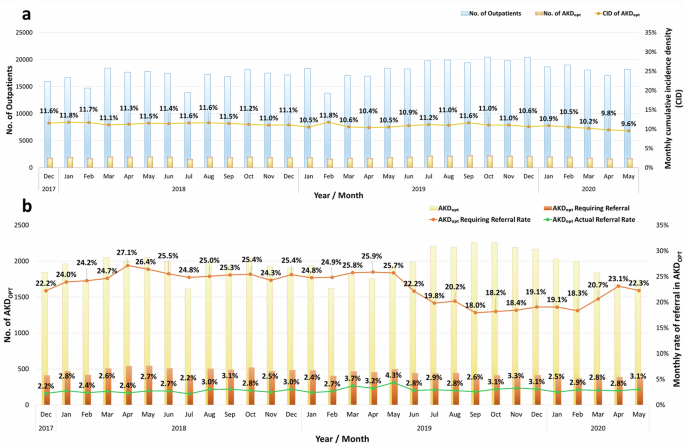
a Monthly occurrence (yellow bars) and cumulative incidence (orange line) of AKDOPT. b Monthly occurrence (orange bars) and rate of AKDOPT requiring nephrology clinic referral (red line), in addition to rate of actual nephrology clinic referral in 1 month (green line). The numerical data used in calculating the incidence were provided in Supplementary Data 2. AKDOPT acute kidney disease in outpatient settings, CID cumulative incidence density, ESKD end-stage kidney disease.
Of the 79,838 eligible outpatients (study population), 12,510 (15.7%) were identified by the AKIDS as having AKDOPT, with 81.0% of them having stable AKDOPT and 19.0% having deteriorating AKDOPT. Compared with patients without AKDOPT, those with AKDOPT were older, were more likely to be a former or active tobacco smoker or alcohol drinker, and had a higher burden of comorbidities such as diabetes and hypertension (Table 1). Patients with AKDOPT were more likely to have an advanced CKD stage (eGFR <60 mL/min/1.73 m2) (18.3% vs 10.5%), had higher blood urea nitrogen and pooled urine albumin-to-creatinine ratio levels but lower serum albumin and hemoglobin levels than did those without AKDOPT (Table 1 and Supplementary Data 4). Because the setting of the S-Cre measurements used to screen for AKDOPT could only be verified if the measurements were from the on-site electronic medical records and because the inclusion of S-Cre from inpatient measurements may interfere the AKDOPT detection, we provided the distribution of S-Cre source. Only 45.2% of the study population had their maximum and minimum S-Cre measurements solely from the outpatient setting, 20.9% from inpatient and 34% from other institutions via the NHI Health Information Exchange (Table 1). The patients with AKDOPT had significantly higher 1-year CKO (12.4% vs. 0.5%), all-cause mortality (8.2% vs. 1.4%), and de novo CKD-ND rates (7.8% vs. 1.6%) than did those without AKDOPT.
Associations of AKDOPT with CKO and all-cause mortality
During the 1-year follow-up, 1942 patients died and 1858 had CKO (96 had ESKD; 1702 had a > 40% decrease in eGFR; 783 had a twofold increase in S-Cre levels; not mutually exclusive). The incidence of 1-year CKO was notably higher in patients with AKDOPT than in those without AKDOPT (12.77 vs 0.42 per 1000 person-months); the adjusted absolute risk was 79 (95% CI 78.9–79.1) per 1000 persons. The corresponding difference for deteriorating AKDOPT was even higher, reaching 109.7 (95% CI 109.5–109.9) per 1000 persons (Table 2). The 1-year mortality rate was significantly higher in patients with AKDOPT than in those without AKDOPT (7.12 vs 1.15 per 1000 person-months); the adjusted absolute risk was 25.3 (95% CI 25.2–25.3) per 1000 persons. The absolute risk of mortality was higher in patients with stable AKDOPT than in those with deteriorating AKDOPT. Moreover, the aHRs for 1-year CKO and mortality in the AKDOPT group relative to the non-AKDOPT group were 16.2 (14.2–18.5) and 2.6 (2.4–2.9), respectively (Table 2). The aHRs for 1-year CKO and mortality in the deteriorating-AKDOPT group relative to the non-AKDOPT group were 22.7 (19.5–26.4) and 2.1 (1.8–2.6), respectively; the same aHRs in the stable-AKDOPT group relative to the non-AKDOPT group were 14.3 (12.5–16.4) and 2.8 (2.5–3.1), respectively. Among patients without baseline CKD, the corresponding aHRs for 1-year de novo CKD-ND in the AKDOPT, deteriorating-AKDOPT, and stable-AKDOPT groups relative to the non-AKDOPT group were 3.5 (3.1–3.9), 4.1 (3.5–4.8), and 3.3 (2.9–3.7), respectively. For each outcome, the time-to-event curves were significant different between AKDOPT and non-AKDOPT groups, as well as across AKDOPT subgroups (Fig. 3a–c and Supplementary Fig. 6a–c).
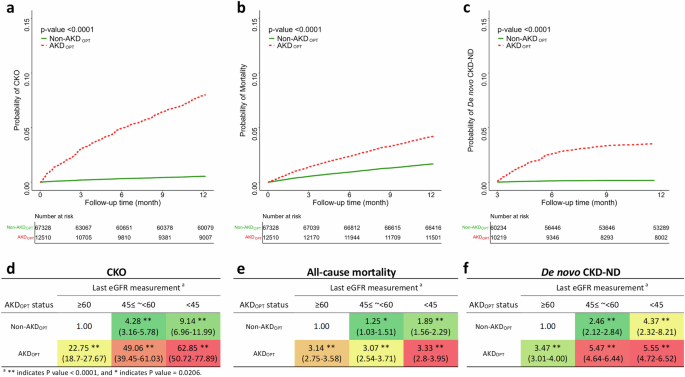
a–c Adjusted 1-year time-to-event curve for CKOs, all-cause mortality, and de novo CKD, respectively, categorized according to AKDOPT status. Variables used for adjustment in the Cox proportional hazards models are described in Model 3. The sample sizes are 79,838 for (a, b) and 70,453 for (c). d–f Corresponding risk matrix accounting for the ultimate eGFR and AKDOPT for CKOs, all-cause mortality, and de novo CKD, respectively. The associations of AKDOPT with the risk of outcomes were evaluated using separate multivariable Cox proportional hazards models. The number represents the aHR (95% CI) of each outcome of interest from Model 3 based on the ultimate eGFR and AKDOPT (lower aHRs in green and higher aHRs in red). aHR adjusted hazard ratio, AKDOPT acute kidney disease in outpatient settings, CI confidence interval, CKD chronic kidney disease, CKOs composite kidney outcomes, eGFR estimated glomerular filtration rate, ND nondialysis.
Of patients who were younger than 65 years or those were free from comorbidities such as diabetes, hypertension, or CKD at baseline, having AKDOPT was associated with a significantly higher risk of 1-year CKO, mortality, and de novo CKD-ND (Supplementary Fig. 7). The risk matrix demonstrated that the aHR for each outcome exhibited a gradient increase from low-risk (non-AKDOPT and ultimate eGFR of ≥60) to high-risk patients (AKDOPT and ultimate eGFR of <45) (Fig. 3d–f and Supplementary Fig. 6d–f).
We conducted various sensitivity analyses to ensure the robustness of our results. The aHR and absolute risks from these analyses aligned with our main findings under different conditions: (1) without multiple imputation (Supplementary Table 4), (2) with diagnostic S-Cre measurements exclusively from CMUH’s outpatients (Supplementary Table 5) and with at least one diagnostic S-Cre from CMUH’s outpatients (Supplementary Table 6), () with at least one outpatient S-Cre during follow-up (Supplementary Table 7), (4) with diagnostic S-Cre taken within the standard 90-day AKD diagnostic window (Supplementary Table 8), and (5) with diagnostic S-Cre taken from CMUH’s outpatients within 90-day window (Supplementary Table 9). By applying the most stringent definition for AKDOPT, we found larger effect sizes for the aHRs and adjusted absolute risks (Supplementary Table 9), which implies that our original definition might have underestimated the clinical impact of AKDOPT. For the 87,426 patients initially excluded because of an unknown AKDOPT status, we adopted the CMUH’s median outpatient S-Cre levels (adjusted for age, sex, and CKD status) as the baseline S-Cre. The association of AKDOPT with 1-year CKO, mortality, and de novo CKD remained significant, albeit with a reduced effect size (Supplementary Table 10).
Recovery pattern of AKDOPT and nephrology follow-up
Of the patients with AKDOPT, 23.4%, 70.0%, and 41.6% experienced recovery to their baseline S-Cre levels (absolute recovery), recovery to ≤0.2 mg/dL above baseline levels, and recovery to ≤1.1 times the baseline levels within 1 year, respectively (Table 1). However, compared with the patients with stable AKDOPT (22.4%), those with deteriorating AKDOPT had a higher absolute recovery rate (27.1%). This may be attributed to the fact that patients with deteriorating AKDOPT were more likely to be regularly followed by nephrologists (12.2% vs 7.0%) and were follow-up sooner (23 days vs 48 days), compared to those with stable AKDOPT. Among the patients with CKD at baseline, 22.4%, 19.3%, and 29.4% of the patients with AKDOPT (all), stable AKDOPT, and deteriorating AKDOPT had CKD stage progression, respectively (Table 1). The nephrology follow-up rate within 90 days following the index date was 2.7%, 2.2%, and 4.9% for the patients with AKDOPT, stable AKDOPT, and deteriorating AKDOPT, respectively.
link






:max_bytes(150000):strip_icc()/VWH-GettyImages-2157903338-69370a8ef92e449b8958c22cab26dd28.jpg)