Study design
This single-center, non-randomized, longitudinal feasibility study was conducted from May 16th to September 13th, 2024, to evaluate feasibility, safety, and describe trends in potential efficacy of a sailing-based rehabilitative intervention for individuals with RSDs.
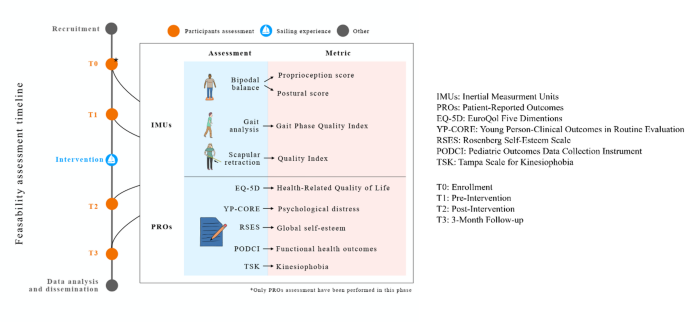
The study design was chosen to prioritize analysis of feasibility metrics while addressing the challenges of conducting research with small, and heterogeneous populations affected by RSDs. The intervention and assessments followed the CONSORT guidelines for feasibility trials (Appendix A)25. A visual summary of the study’s timeline and participants assessment is provided in Fig. 1.
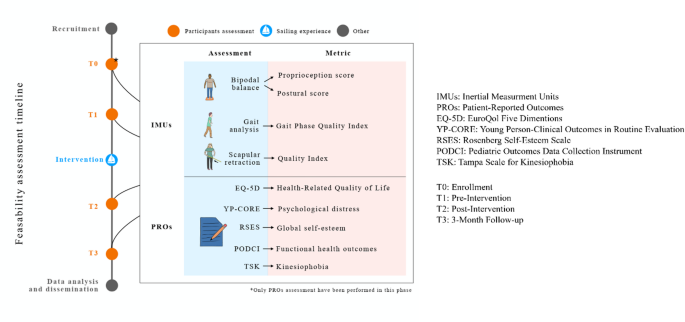
Feasibility study timeline and participants assessment from recruitment to three-month follow-up.
All data were managed using the REDCap electronic data storage tool hosted at Yale University. REDCap’s real-time data validation, automated audit trails, and centralized management features ensured data integrity across multiple time points, particularly given the complexity of managing repeated measures in a longitudinal study26.
Ethical approval was obtained from the Local Ethical Committee, Comitato Etico Area Vasta Emilia Centro (CE-AVEC), under protocol number 115/2024/Sper/IOR. The study was registered on ClinicalTrials.gov (NCT06397443) and conducted in accordance with the 1964 Declaration of Helsinki and its subsequent amendments.
Setting
The study was conducted across three sites: enrollment (at T0) and three-month follow-up assessment (T3) were performed at IRCCS Istituto Ortopedico Rizzoli (IOR), national referral centre for RSDs, based in Bologna, Italy; sailing sessions were held at the port of Marina di Ravenna, Italy; and ‘Palazzo Manzoni’ in San Zaccaria (Ravenna, Italy) served as the accommodation site, hosting the pre- and post-intervention (T1 and T2) evaluations.
Participants’ recruitment
Participants were recruited and screened from April 10th to May 10th, 2024, using a combined approach, including direct engagement during outpatient visits at the Department of Rare Skeletal Disorders at IOR and through outreach to the national rare disease community, with social media initiatives and patient advocacy networks, in collaboration with UNIAMO-Federazione Italiana Malattie Rare (UNIAMO-FIMR), the Italian umbrella patients advocacy organization, who played an essential role in the study’s conceptualization, planning, execution, and dissemination.
Eligibility criteria included: (a) age of 12 years or older; (b) a confirmed diagnosis of a rare skeletal disorder; (c) the ability to engage in physical activities with adaptations; and (d) no surgical interventions within the six months before enrollment. These criteria were selected to ensure a balance between homogeneity for meaningful analyses and practical inclusivity given the rarity of the conditions.
Exclusion criteria included: (a) ongoing evaluation for a differential diagnosis; (b) recent surgical interventions (< 6 months); (c) fractures or musculoskeletal injuries (< 12 months); (d) conditions contraindicating marine environments or sailing activities; (e) absence of a rare skeletal disorder (i.e., healthy individuals); or (f) refused to provide informed consent.
Written informed consent was obtained from participants aged 18 years or older, and parental/guardian consent was secured for minors.
Sample size
Consistent with FDA Rare Disease Guidance (2023), a sample size of eight participants was selected to prioritize feasibility outcomes (e.g., 85% power to detect adherence rates > 75% at α = 0.10)27. This approach aligns with recommendations for pilot studies in rare populations. Small cohorts are necessary in early-phase studies due to limited recruitment capacity and patient heterogeneity; as noted by Mitani et al. (2020) and Videnovic et al. (2023), small sample sizes are scientifically and ethically justified, providing reliable feasibility data to inform later for larger, confirmatory studies28,29.
Intervention
The sailing-based intervention (Fig. 2) was conducted through a collaboration between IOR research team, Euleria srl Società Benefit, and Marinando Ravenna ODV, a charitable organization based in Marina di Ravenna. This organization advocates sailing and navigation as effective means of promoting social integration, emphasizing the values of perseverance, discipline, respect for others, inclusivity, and active participation. The sailing sessions took place at the ‘Marinara’ port in Marina di Ravenna, with each session lasting approximately five hours. Sessions were scheduled from the morning to the afternoon, starting with a brief overview of the daily activities, followed by the division of participants into two groups of equal sizes.

Timeline and activities of the sailing-based rehabilitative intervention. The timeline and structure of the sailing-based rehabilitation intervention are summarized in this figure. The program covered five days, starting with an orientation session and a pre-intervention assessment (T1) on Day 1. Over the next three days (Days 2–4), participants engaged in daily sailing sessions, which included morning briefings to set objectives, practical sailing activities, and debriefing sessions to reflect on the experiences. On the final day (Day 5), a feedback session and post-intervention assessment (T2) were conducted to gather participants’ perspectives and to evaluate both physical and psychological outcomes. A follow-up at three months was also planned to assess the sustainability of the intervention’s effects.
Over a five-day period, participants engaged in three sailing sessions, each lasting five hours. The first and last days were dedicated to physical and psychological data collection, while the intermediate days included sailing activities combined with structured debriefing meetings. Participants were accommodated at the ‘Palazzo Manzoni’, which served as the site for daily debriefing activities, and hosted the full program on the first and last day. On the first day (May 27th, 2024), participants attended an explanatory session, where they were introduced to the Marinando skippers and volunteers, received basic sailing instruction, and were briefed on safety procedures. On the final day (May 31st, 2024), participants took part in an extended debriefing discussion, offering detailed feedback on their emotional, cognitive, and experiential responses to the intervention. This session lasted approximately two hours.
Two 10-meter sloop-rigged sailing yachts (Oasis 33s model), “Gaia” and “Rolling Black”, adapted to accommodate individuals with disabilities and special needs, were used for the sailing sessions (Fig. S1). These boats were skippered by Marinando-certified instructors. Volunteers from Marinando Ravenna ODV supported the participants throughout the activities. Participants actively rotated through various roles on the boat (such as steering, adjusting sails, and assisting with navigation), under the guidance of the skipper. The final session included a friendly race between the two boats. Each sailing session concluded with a one-hour debriefing session conducted by clinical psychologist research assistant, allowing participants to reflect on their experiences, discuss challenges faced, and provide feedback.
In case of adverse weather conditions, contingency plans were implemented to ensure both the safety and engagement of participants. Activities were either rescheduled or adapted while maintaining the treatment aims of the program.
Daily transportation between ‘Palazzo Manzoni’ and the ‘Marinara’ port was thoughtfully arranged by the ‘Pubblica Assistenza Paolina’ of Imola (Bologna, Italy), a public assistance service, ensuring continuous logistical support and participant safety throughout the program.
The intervention adhered to the Template for Intervention Description and Replication (TIDieR, Appendix B), ensuring detailed documentation for replicability30.
Measures
Demographic and clinical characteristics
Baseline demographic and clinical characteristics, including age, gender, educational level, participation in sports, disease type, anthropometric measurements (height, weight, and BMI), physical impairments, and mobility status, were collected during the enrollment visit at IOR (T0). All assessments were conducted by the physical medicine and rehabilitation team specializing in RSDs, using a study-specific Research Report Form (Appendix C).
Primary outcomes: feasibility and safety
Feasibility was evaluated following Bowen et al. (2009), which fits to this study’s context31. Five core parameters were assessed: recruitment, retention, compliance, adherence, and acceptability, with thresholds based on existing literature27,32.
Recruitment was the proportion of eligible participants approached and who consented, with a threshold of ≥ 80%. Retention reflected participants completing the intervention and assessments, targeting ≥ 75%. Compliance was measured by attendance, with satisfactory compliance set at ≥ 75% of sessions. Adherence was defined as total sailing hours completed relative to the planned program, with ≥ 75% completion deemed satisfactory. Acceptability was assessed post-intervention (T2) using a 5-point Likert scale evaluating agreement with the statement, “I have been happy with the things I have done,” from 0 (“Not at all”) to 4 (“Most or all the time”), with a mean score ≥ 3 indicating acceptability.
Safety was monitored after each sailing session using a checklist documenting adverse events, duration, premature discontinuation, and medications. A standardized approach tracked symptom progression and new adverse effects.
This multidimensional assessment comprehensively evaluated the study’s feasibility across key metrics.
Secondary outcomes: health-related quality of life (HRQoL), psychological well-being, and physical functioning
HRQoL and psychological well-being were assessed at all time points (T0 to T3) using validated Italian versions of standardized instruments33,34,35,36,37. A clinical psychology research assistant specializing in RSDs and affiliated with IOR conducted the assessments with paper-based forms.
The EQ-5D is a standardized generic instrument for assessing HRQoL. This study employed the EQ-5D-5 L version for adults (≥ 16 years), following EuroQol guidelines, which allow use from age 1238. The questionnaire evaluates five dimensions: mobility, self-care, usual activities, pain/discomfort, and anxiety/depression, each rated on five severity levels. A summary Index Value (IV) was assigned using the Italian EQ-5D-5 L value set40. Health profiles range from the best (11111) to the worst (55555), with IV scores from 1 (perfect health) to 0 (death-equivalent), and negative values for “worse than death.” Participants also rated their health on a visual analog scale (VAS) from 0 to 100, with higher scores indicating better overall health status.
The PODCI assesses functional health outcomes in pediatric and adolescent musculoskeletal conditions41. It includes 86-item across six scales: Upper Extremity, Transfer and Basic Mobility, Sports and Physical Function, Pain/Comfort, Happiness, and Global Function. Scores range from 0 to 100, with higher values indicating better function. It provides a comprehensive measure of physical ability, pain, and psychosocial satisfaction.
The RSES measures global self-esteem in individuals aged ≥ 12 years42. It includes 10 items rated on a 4-point Likert scale, assessing positive (e.g., “I feel I am a person of worth”) and negative self-esteem (e.g., “At times, I think I am no good at all”). Scores range from 10 to 40, with higher values indicating greater self-esteem.
The YP-CORE assesses psychological distress and well-being in youth16. It consists of 10 items rated on a 5-point Likert scale (0–4), covering emotional well-being, interpersonal functioning, and coping. Scores range from 0 to 40, with higher values indicating greater distress.
The TSK evaluates fear of movement or re-injury due to pain43. The 13-item Italian version, rated on a 4-point Likert scale (1–4), measures harm and activity avoidance. Scores range from 13 to 52, with higher values indicating greater kinesiophobia. It is validated for musculoskeletal and chronic pain populations37.
Physical functioning was assessed from T1 to T3 using objective measures developed in collaboration with biomedical engineers and bioinformatician specializing in RSDs, affiliated with IOR and Euleria Health, a Benefit Company specializing in digital rehabilitation solutions. All assessments were supervised by the physical medicine and rehabilitation team and conducted according to a standardized physical functioning exercises protocol (Appendix D).
The IMUs are wearable, non-invasive devices that provide objective data on movement patterns, including mobility, proprioception, and posture44. They offer quantitative measurements that, along with self-reported outcomes, enable a comprehensive assessment of physical improvement. In this study, five IMUs and a pressure board were integrated with dedicated software (Euleria Lab, Euleria srl, Rovereto, Italy). Both systems communicated with the software via Bluetooth Low Energy (BLE), and operated at a 60 Hz sampling frequency, enabling synchronized data acquisition and real-time visualization (Fig. 3). The IMU system has an angular resolution of 0.1° and a dynamic accuracy within ± 2°, thereby meeting the threshold recommended for clinically relevant motion analysis, particularly in monitoring upper-limb movements45,46. The IMUs were positioned on specific anatomical landmarks with adjustable elastic bands, as detailed below. Calibration was performed before each assessment, requiring participants to stand still for three seconds while wearing the IMUs, and, when specified, standing on the pressure platform.
Three primary assessments evaluated mobility using IMUs:
-
(a)
Bipodal balance: a single IMU at the sternum level was used to estimate postural stability and the Center of Mass (COM), while the Centre of Pressure (COP) trajectory was derived from the pressure board data as participants stood for 30 s. The test was conducted with both eyes open and closed to assess proprioception, with the eyes-closed condition evaluating reliance on vestibular, and somatosensory inputs in the absence of visual feedback.
-
(b)
Gait analysis: five sensors placed on the feet, tibias, and trunk measured the gait cycle during straight walking. Gait phases were compared to standard references to detect asymmetrical or anomalies.
-
(c)
Arm exercises: participants performed bilateral and unilateral scapular retraction (isometric and repetitive) and overhead lateral shifts while wearing five IMUs on the trunk, wrists, and humeri. These controlled the Euleria Lab exergame and collected kinematic data.
Performance was quantified using:
-
I.
In-game score: The “Arm Quality Index” (AQI), calculated within Euleria Lab software, measured adherence to optimal movement trajectories.
-
II.
Raw and derived scores: Additional metrics included the Gait Phase Quality Index (GPQI), Proprioception Scores, and Postural Scores.
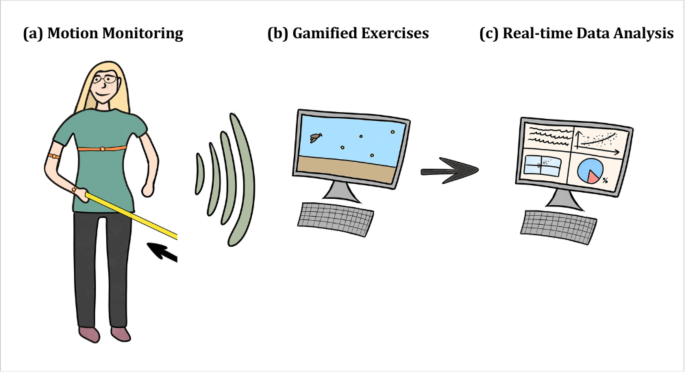
Workflow for IMU-based motion monitoring, gamification, and data analysis. This figure presents a sensor-based telerehabilitation workflow designed to enhance rehabilitation outcomes. The system incorporates three key components: (a) motion monitoring, where wearable sensors capture real-time motion data during patient movements; (b) gamified exercises, employing interactive tasks to promote patient adherence and motivation; and (c) real-time data analysis, delivering immediate feedback and generating clinically relevant insights to support data-driven decision-making for personalized rehabilitation interventions.
Statistical analysis
Descriptive statistics, including median, minimum and maximum, mean, standard deviations, and frequencies, were used to illustrate the study population and summarize feasibility, and safety outcomes.
HRQoL and psychological well-being outcomes were calculated according to the developers’ guidelines.
Physical functioning outcomes were assessed using specific quantitative metrics designed to evaluate proprioception, postural control, gait and arm quality, which are critical for understanding the impact of the intervention.
The Proprioception Score quantifies proprioceptive control by integrating trunk and COP variability. Trunk position was recorded using a sternum IMU, while COP position was measured via a pressure board. Both signals were synchronized at 60 Hz using Euleria Lab software (Euleria srl, Rovereto, Italy).
The score was calculated as:
$$\:Proprioception\:Score=\:\frac{1}{{\sigma\:}_{t}+{\sigma\:}_{COP}}\times\:100$$
where σt and σCOP represent the standard deviations of the distribution of the trunk and COP positions, respectively. Lower variability of trunk and COP indicates higher proprioceptive control, reflected by a higher Proprioception Score47,48.
The Posture Score assesses posture control by evaluating the alignment between trunk and COP. Trunk position was recorded via the sternum IMU, and COP via the pressure board, with both signals synchronized at 60 Hz.
The score was calculated as:
$$\:Postural\:Score=\frac{1}{{\overline{D}}_{\left(t-COP\right)}}\times\:100$$
where \(\:{\overline{D}}_{\left(t-COP\right)}\:\)is the average Euclidean distance between trunk and COP positions. Smaller distances indicate closer trunk-COP alignment, corresponding to higher posture control and a higher Posture Score47,48.
The AQI quantifies the performance of the patient during the gaming experience, and it expressed as a percentage.
The GPQI total was calculated using the formula:
$$\:{GPQI}_{tot}=\sqrt{\sum\:_{i=1}^{4}{\left({P}_{Ri}-{r}_{i}\right)}^{2}+\sum\:_{i=1}^{4}{\left({P}_{Li}-{r}_{i}\right)}^{2}}$$
where P represents the observed proportion of time spent in each phase for both the right (R) and left (L) foot and the reference value r for each ith phase of the gait cycle. The reference values (r) correspond to normative gait timing in healthy subjects: heel strike 7%, full stance 39%, heel-off 16%, and swing 38%. The squared differences between the observed and reference values are summed across the four phases for both feet. The square root of this sum yields the GPQI, which reflects how the individual’s gait deviates from the normal pattern across all phases of the gait cycle. Higher GPQI values indicate greater deviation from normal gait, capturing both inter-limb asymmetries and overall phase timing differences.
Changes over time were analyzed using the Wilcoxon signed-rank test, selected for its robustness with small sample sizes and non-normal data distributions. Statistical significance was set at p < 0.05 and p < 0.10, recognizing the exploratory nature of this feasibility study and the inherent limitations of statistical power in small sample sizes. In addition, a significance of 0.10 < p < 0.15 was applied to highlight potential trends warranting further investigation. Data analysis was performed using R software version 3.6.3 (The R Foundation for Statistical Computing, Wien).
link





:max_bytes(150000):strip_icc()/VWH-GettyImages-2157903338-69370a8ef92e449b8958c22cab26dd28.jpg)