Patients
Family cooperation
During interviews, five medical experts mentioned that families are often overly eager, expecting patients to regain mobility, leading to the common occurrence of “over-rehabilitation.” This refers to a situation where patients undergo excessive or intensive rehabilitation efforts, often driven by unrealistic expectations from families or caregivers. They believed that this “over-rehabilitation” not only reduces the patient’s independence, causing excessive reliance on the family and affecting their ability to participate in rehabilitation activities and self-management, but also increases pressure on the patient. This may lead to frustration or an inability to meet high expectations, causing resistance and negative emotions toward the rehabilitation plan.
“The role of family members is twofold. Financial and psychological support can enhance patients’ adherence to rehabilitation, but excessive care can also be a hindrance to rehabilitation. For example, helping patients dress or feed them can create dependency, affecting the patients’ rehabilitation expectations. Allowing patients to do what they can for themselves leads to better rehabilitation outcomes.” — Associate Professor of Rehabilitation Medicine, male, 49 years old.
Economic pressure
Several medical experts have highlighted that a patient’s financial situation significantly affects their rehabilitation adherence. At the individual level, economic pressure can manifest in many forms, such as job loss, financial distress, and difficulty paying bills. With substantial economic pressure, patients may struggle to adhere to planned rehabilitation activities, face challenges in purchasing necessary medications, or have difficulty accessing essential rehabilitation resources (such as physical therapy or rehabilitation equipment). Economic pressure can lead to anxiety and depression, further promoting the development of complications and comorbidities.
“Currently, hyperbaric oxygen therapy, acupuncture, electrotherapy, and physical therapy are the main methods of patient rehabilitation. Hyperbaric oxygen therapy is more effective but more expensive. Patients in Shanghai have agricultural insurance (high reimbursement rate), so most can accept hyperbaric oxygen therapy. However, most patients from other regions, facing economic pressure, do not accept hyperbaric oxygen therapy, making up about 15% of patients.” — Deputy Chief Physician of Neurology, female, 44 years old.
Hospitals
Department collaboration
Most medical experts also believed that when a patient has had a stroke and is admitted to the cerebrovascular or neurology department during the onset period, the involvement of rehabilitation doctors can aid in functional recovery during the treatment of the primary disease. Unfortunately, many rehabilitation medical experts suggest that departmental collaboration is not straightforward and that the involvement of rehabilitation doctors is often not timely.
“It often happens that patients are hospitalized in the neurology department, where they receive clinical treatment from them. At the end of the initial consultation, the neurology department did not notify the rehabilitation doctors for a consultation, so the rehabilitation doctors were not involved in the treatment process. Moreover, the patient went home directly after treatment in the neurology department.” — Deputy Director of Neurology, Chief Physician, Female, 44 years old.
Hospital investment
Most medical experts indicated that most hospitals, especially community hospitals, lack rehabilitation doctors, making it difficult to understand and meet patients’ needs promptly and adequately. This results in poor medical outcomes and patient experiences, leading them to mistakenly believe that rehabilitation has little impact on their health. Furthermore, with the general shortage of beds in rehabilitation departments, patients find it difficult to secure beds and receive timely formal rehabilitation.
“Community professional staff are severely lacking, and many community hospitals do not have rehabilitation doctors. Community hospitals also face the problem of having few and unprofessional therapists.” — Deputy Director of Neurology, Chief Physician, Female, 44 years old.
“I hope that hospitals can improve their ward facilities. Currently, rehabilitation department wards are crowded, with few bathrooms, and overall poor conditions.” — Chief Physician of Rehabilitation Department, Female, 60 years old.
Training of rehabilitation talent
Research found that most hospitals lack adequate training for rehabilitation doctors, and the training content is not standardized. Because few practicing physicians have a degree in rehabilitation medicine, most rehabilitation therapists require professional training to improve their treatment levels to meet the minimum treatment standards.
“The professional level of rehabilitation therapists needs to be improved, especially among young people. Therefore, hospitals should regularly train rehabilitation therapists. Hospitals can set up regular training departments for rehabilitation workers to enhance the professional ability of personnel.” — Chief Physician of Rehabilitation Department, Male, 58 years old.
Society-related factors
Government support
Almost all medical experts advocate for government policy inclinations and financial support to expand the promotion of rehabilitation medicine knowledge and increase public awareness. A higher medical insurance reimbursement rate boosts patients’ enthusiasm for rehabilitation and allows them to actively receive treatment without excessive financial burdens.
“The government should do more publicity to raise the awareness of rehabilitation throughout society. Moreover, the government should correct the professional qualifications of rehabilitation therapists. For example, the Ministry of Human Resources and Social Security recently classified rehabilitation therapists as social service workers, similar to catering service workers. This cannot guarantee the identity and social status of rehabilitation therapists and may negatively affect their work motivation.” — Associate Professor of Rehabilitation Department, Male, 49 years old.
Social awareness
According to medical experts, social awareness impacts rehabilitation compliance in three ways. First, it influences whether patients feel support from family, friends, and the community. Second, it involves interactions between patients and rehabilitation teams. Third, social awareness can shape expectations and attitudes of others toward the rehabilitation of patients who have had a stroke.
“Overall, the social awareness of rehabilitation remains low. Most people mistakenly understand rehabilitation as physical therapy session, a massage, or undergoing some form rehabilitation, thus necessitating publicity and education for the public (including clinical doctors).” — Associate Professor of Rehabilitation Department, Male, 49 years old.
Accessibility of medical resources
Research found that high medical resource accessibility makes it easy for patients to obtain the necessary rehabilitation equipment and receive guidance from healthcare professionals. Continuous rehabilitation encourages patients to actively participate in treatment, thereby enhancing their confidence in the process.
“A 60-year-old aunt with level three hemiplegia was brought to the hospital by her family for rehabilitation. Upon admission, she was only being fed through a nasal tube. Based on the evaluation of her swallowing and limb functions, the prognosis should be good. In about half a month, her condition would significantly improve. However, the patient was discharged after only a week, mainly due to financial conditions and her children’s need to return to work in nearby prefecture-level cities, which lack specialized rehabilitation hospitals.” — Chief Physician of Rehabilitation Medicine, Female, 36 years old.
Establishing a three-tier rehabilitation network
Some medical experts point out that three-tier rehabilitation, such as community and home rehabilitation, can be more effective, where community hospitals can also undertake certain rehabilitation work. Unfortunately, Most medical experts indicated that despite significant improvements in constructing the three-tier rehabilitation system, it falls short of expectations.
“Society lacks barrier-free facilities, so regardless of how well patients rehabilitate, many eventually become disabled. If barrier-free facilities are not increased, these patients’ social participation will be very low. In Japan, there are taxis specifically for disabled people in wheelchairs, allowing them to independently use transportation to visit doctors. These facilities help patients reintegrate into society.” — Deputy Chief Physician of Neurology, Female, 44 years old.
Establishing industry standards and norms
Research found that rehabilitation medicine lacks unified scientific standards in China and globally. As the saying goes, “Three parts treatment, seven parts care,” but regrettably, the current structure of rehabilitation personnel in China cannot meet the standards of a continuous care model. Most medical experts indicated that one of the main reasons for this is the lack of professional certifications and commissioned training in the rehabilitation medical system.
“The rehabilitation treatment system lacks systematic and standardized approaches. The government should establish standardized referral mechanisms (setting corresponding standards), unify personnel requirements, clarify unified management models (such as medical documents), and establish supervision and regulatory mechanisms for the medical process.” — Chief Physician of Rehabilitation Department, Male, 50 years old.
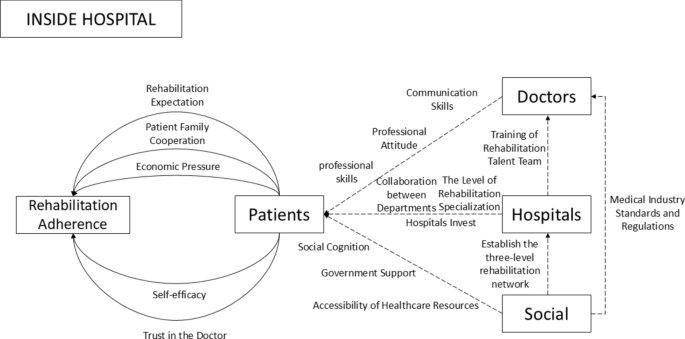
According to the above analysis, the facilitators to hospital-based rehabilitation include key facilitators for stroke rehabilitation adherence include patients’ positive rehabilitation expectations, strong self-efficacy, and trust in doctors. Higher cognitive abilities enable patients to set realistic goals, while psychological resilience helps them overcome challenges. Effective doctor-patient communication and physicians’ professional attitudes enhance treatment plans. Government support through policies and insurance coverage, along with improved social awareness and accessible medical resources, further promote rehabilitation adherence. Meanwhile, the barriers to hospital-based rehabilitation involve patients’ unrealistic expectations due to low cognitive levels, leading to mistrust in doctors. Limited healthcare resources, financial constraints, and lack of standardized rehabilitation protocols hinder treatment continuity. Inadequate social awareness and insufficient barrier-free facilities reduce patients’ social participation. Additionally, the absence of professional certifications and training for rehabilitation staff impacts service quality and motivation.
link





:max_bytes(150000):strip_icc()/VWH-GettyImages-2157903338-69370a8ef92e449b8958c22cab26dd28.jpg)